Knowledge, attitudes, and practices regarding metabolic associated fatty liver disease (MAFLD) in elderly patients
Elderly patients with MAFLD demonstrated insufficient knowledge, unfavorable attitudes, and limited proactive practices toward disease management, highlighting a significant gap in their understanding and engagement with self-care practices. These findings underscore the urgent need for targeted educational interventions and structured health promotion programs aimed at enhancing knowledge, fostering positive attitudes, and encouraging evidence-based practices among elderly patients to improve disease outcomes and quality of life.
This study targeted on elderly patients aged 60 and above who suffer from MAFLD. The lower age limit of 60 years was chosen to account for generational differences in disease cognition and health behaviors, particularly in the context of MAFLD as a hepatic manifestation of metabolic syndrome. Elderly patients often manage multiple chronic conditions, such as cardiovascular disease and diabetes, which influence disease management. Additionally, while MAFLD onset occurs earlier in men, the incidence and severity of metabolic disorders tend to converge with age, particularly after 45 years21,22. Setting the threshold at 60 minimized age-related confounding, allowing for a more precise evaluation of gender differences in KAP. The limited awareness of MAFLD’s progression to cirrhosis or cancer (29.95% unclear; K5) may hinder early recognition of systemic risks associated with MAFLD, as highlighted by Pipitone et al.21,22, who characterized MAFLD as a multisystem disease linked to cardiovascular and oncological complications. This gap underscores the need for interventions addressing both hepatic and extrahepatic risks through comprehensive patient education.”
This study sheds light on the substantial gaps in KAP among elderly patients with MAFLD, revealing a troubling lack of awareness, negative attitudes, and limited engagement in proactive health behaviors. These findings align with broader patterns observed in similar populations, where chronic metabolic conditions are often accompanied by insufficient understanding and suboptimal disease management23. For instance, studies have shown that among elderly patients with diabetes, only 35–50% exhibit adequate knowledge about disease management, which significantly affects their ability to adhere to treatment plans and engage in preventive practices23. Similarly, a study on cardiovascular diseases revealed that less than 40% of elderly patients were aware of the importance of lifestyle modifications, such as diet and exercise, in improving disease outcomes. In particular, the knowledge scores in this study highlight pervasive misconceptions about MAFLD, including limited awareness of its risk factors, symptoms, and potential complications. These results are consistent with studies showing that the elderly population frequently underestimates the severity of chronic liver diseases, often perceiving them as non-urgent or inevitable consequences of aging24.
The low practice scores observed in this study further reflect a broader challenge in translating knowledge and attitudes into actionable health behaviors. Previous studies in populations with chronic conditions, such as diabetes and cardiovascular diseases, have reported similar barriers to the adoption of lifestyle modifications, often attributing them to a lack of tailored support, inadequate follow-up, and insufficient health education25. The limited engagement in regular exercise and dietary adjustments noted among participants mirrors trends reported in other studies of elderly patients, where physical limitations, cognitive decline, and cultural norms regarding aging contribute to low adherence to lifestyle interventions26. Furthermore, the relatively low rates of health promotion and education related to MAFLD in the study population underscore systemic gaps in healthcare delivery, particularly in preventative care and patient education, which are critical for effective disease management27,28.
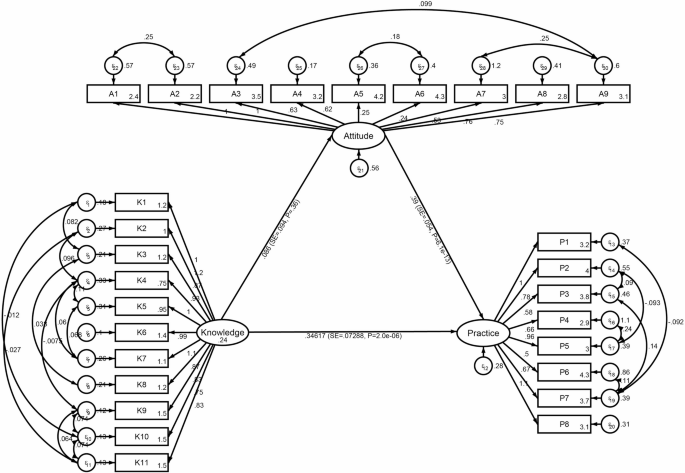
Our findings on the correlations between KAP dimensions are consistent with existing health behavior models, such as the Health Belief Model, which suggests that awareness of a condition influences attitudes and subsequent behaviors29. Similar associations have been observed in studies on chronic diseases, where higher knowledge levels correlate with more proactive self-management behaviors30. However, the moderate correlation strength in our study indicates that knowledge alone may not be sufficient to drive behavior change, underscoring the need for interventions addressing attitudes and behavioral barriers. The structural equation modeling results further highlight the mediating role of attitudes in shaping practice, a pattern observed in studies on other chronic diseases where self-efficacy plays a crucial role31. Although our SEM model demonstrated good fit indices for RMSEA (0.068), TLI (0.877), and CFI (0.895), the SRMR value (0.110) exceeded the commonly accepted threshold of 0.08. This discrepancy may be attributed to several factors. First, the complexity of KAP relationships in elderly populations with chronic conditions like MAFLD often involves unmeasured confounding variables that influence the residual correlations between observed indicators32. Second, the heterogeneity in our elderly sample regarding disease duration, comorbidities, and cognitive function may have introduced additional variance not fully captured by our model specification33. We tested alternative model specifications including additional demographic variables and interaction terms; however, these more complex models yielded poorer overall fit indices. The current model represents the most parsimonious solution that balances theoretical coherence with empirical fit. This finding aligns with previous KAP studies in chronic disease populations where perfect model fit is challenging to achieve due to the multifaceted nature of health behaviors in elderly populations34. The non-significant indirect effect of knowledge on practice via attitude, as well as the lack of a direct association between knowledge and attitude, partially contradicts the classical linear assumptions of the Knowledge-Attitude-Practice model, which posits that knowledge shapes attitudes, which in turn influence behavior. These findings suggest that in older adults’ self-management of MAFLD, additional mediating variables—such as self-efficacy, social support, or perceived barriers—may play a more critical role in translating knowledge into attitudes and practice35. Future research should explore these alternative mediators by integrating theoretical frameworks, such as the Health Belief Model or Social Cognitive Theory, to better capture the complexities of behavioral change in this population.
The differences observed in KAP scores across demographic and socioeconomic variables highlight important disparities that warrant attention. Participants with higher levels of education exhibited better knowledge and practices, which aligns with broader literature demonstrating that education is a key determinant of health literacy and the ability to navigate complex healthcare systems36. Similarly, income disparities significantly impacted KAP scores, with higher-income individuals demonstrating greater engagement in proactive health behaviors, reflecting well-documented inequities in access to healthcare resources and educational opportunities37.
Age also played a critical role, as older participants were found to have lower knowledge and practice scores, consistent with studies showing that cognitive decline, limited mobility, and reduced access to information often impede effective disease management among the elderly38. These findings underscore the need for targeted interventions that address these disparities, particularly among vulnerable subgroups with lower socioeconomic status or advanced age.
The distribution patterns observed in specific knowledge and attitude items provide further context for understanding these gaps. Items related to the long-term complications of MAFLD, such as its progression to liver cirrhosis or cancer, received particularly low correct response rates, reflecting a broader issue in public health communication about the severity and systemic risks associated with chronic liver diseases. Similarly, the skepticism toward the efficacy of MAFLD treatment observed in attitude responses is consistent with findings from other studies, where patients with metabolic conditions often express doubts about the benefits of medical interventions, possibly due to previous negative experiences or a lack of visible improvements39.
To address these gaps, future educational and interventional programs should incorporate evidence-based strategies tailored to the needs of elderly MAFLD patients.
First, structured health education sessions integrated into routine primary care visits have been shown to enhance patient awareness and improve outcomes. A randomized controlled trial demonstrated that lifestyle interventions including structured education significantly improved histological features of NAFLD40. These sessions should provide clear, actionable information on MAFLD risk factors, symptoms, and management strategies using visual aids, culturally adapted materials, and simplified language to accommodate varying literacy levels41. Second, evidence-based interactive workshops and peer-led support groups can foster engagement and reinforce behavior change, as studies have found that intensive lifestyle modification programs resulted in significant NASH resolution through improved adherence to recommended practices42. Such approaches enable patients to share experiences and receive practical guidance from healthcare professionals while improving clinical outcomes. Third, digital health interventions, such as smartphone applications or telemedicine platforms, could facilitate continuous monitoring and education, particularly for those with mobility limitations43. These tools can provide personalized reminders for dietary adherence, physical activity, and regular medical check-ups. Lastly, targeted public health campaigns emphasizing the importance of early detection and lifestyle modifications should be implemented in collaboration with community organizations to reach a broader audience. By integrating these approaches, healthcare systems can effectively bridge the gap between knowledge and practice, ultimately improving self-management and clinical outcomes in elderly MAFLD patients.
At the individual level, structured behavior changes programs that focus on fostering positive attitudes and building self-efficacy are essential. These could include motivational interviewing techniques and personalized goal-setting interventions aimed at encouraging lifestyle modifications such as regular exercise and dietary adjustments. Drawing from successful chronic disease management programs, such as those for diabetes and cardiovascular health, these interventions could be adapted to the specific needs of MAFLD patients, emphasizing practical strategies for sustainable behavior change44. Healthcare providers should also receive additional training to equip them with the skills needed to effectively communicate with elderly patients, addressing both informational and emotional aspects of care.
Resource allocation must prioritize the development of supportive infrastructure for these interventions. This includes expanding access to affordable diagnostic tools, such as regular liver function tests, and ensuring the availability of multidisciplinary care teams, including dietitians and physical therapists, who can provide tailored support for MAFLD management. Policymakers should consider incentivizing healthcare organizations to adopt these models of care, recognizing the long-term cost-effectiveness of preventative and patient-centered approaches45. Finally, implementing digital health solutions, such as telemedicine platforms and mobile health apps, could further enhance accessibility, particularly for elderly patients with mobility limitations or those in underserved areas. However, these solutions must be designed with user-friendly interfaces and supported by adequate training to ensure their effectiveness and adoption24.
This study has several limitations. First, the cross-sectional design limits our ability to infer causal relationships among KAP variables, as associations do not imply causation. Longitudinal studies are needed to determine how knowledge and attitudes influence long-term behavioral changes. Second, reliance on self-reported data introduces potential biases, including social desirability and recall bias, which may lead participants to overestimate their knowledge or adherence to recommended practices. Future studies could incorporate objective measures, such as clinical assessments or digital health monitoring, to improve data accuracy. Third, as the study was conducted at a single hospital in Shanghai, the findings may not fully represent elderly individuals with MAFLD in different healthcare settings or regions. Fourth, our quality control measures, including the exclusion of participants who failed the trap question or completed the survey too quickly, may have introduced selection bias. While these steps ensured data reliability, they may also have led to the exclusion of individuals with lower cognitive engagement or digital literacy, potentially limiting the generalizability of our findings. Fifth, the SRMR value exceeding the threshold suggests potential unexplained variance, indicating the omission of influencing factors. Attempts to incorporate additional variables led to poorer model performance, suggesting the current model is the best balance between complexity and fit. Future studies should incorporate longitudinal designs and additional variables, such as healthcare access and socioeconomic status, to refine the model and enhance understanding of KAP influences.
In conclusion, elderly patients with MAFLD demonstrated insufficient knowledge, suboptimal attitudes, and a limited engagement in proactive practices related to disease management. These findings highlight the urgent need for targeted educational interventions and awareness campaigns to enhance knowledge, foster positive attitudes, and promote effective practices among elderly patients with MAFLD, thereby improving clinical outcomes and quality of life.
link