New Study Reveals COVID-19 AKI Patients Face Lower Long-Term Kidney Risks
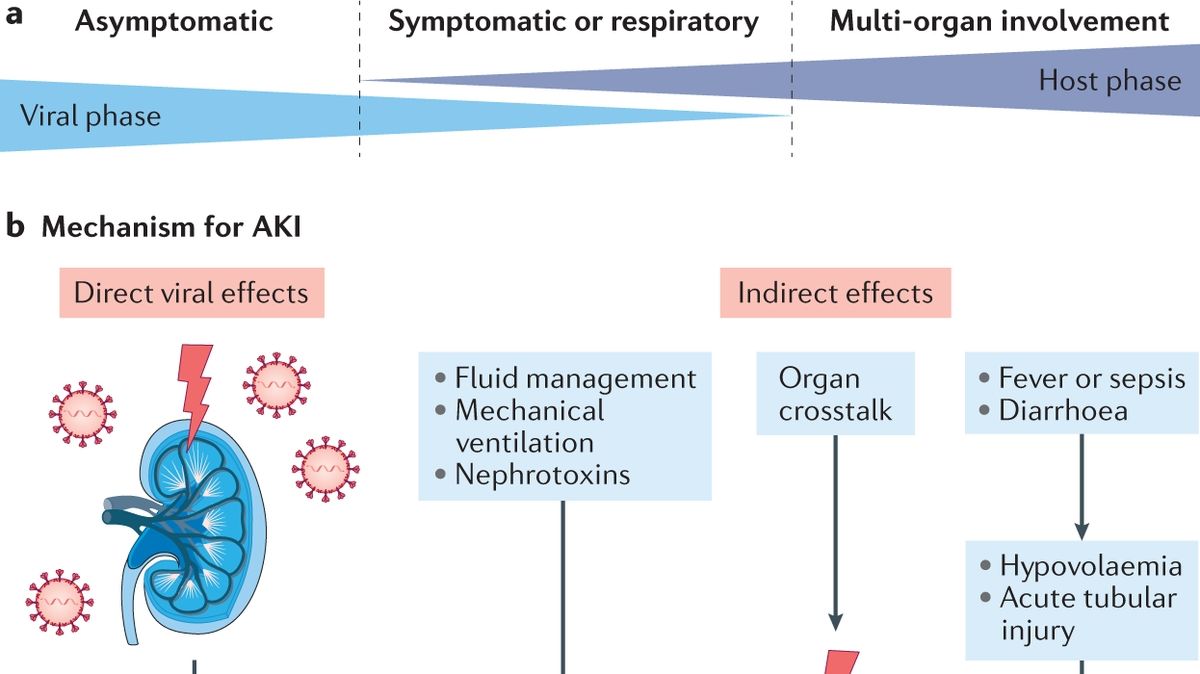
In a breakthrough that is lighting a path of hope through the remnants of pandemic shadows, recent research has provided a significant sigh of relief to COVID-19 survivors and the medical community alike. The crux of the matter lies in understanding the long-term kidney outcomes for patients who suffered from Acute Kidney Injury (AKI) due to COVID-19. Contrary to initial fears, these individuals do not face a higher risk of enduring kidney issues compared to those whose kidney diseases stemmed from other causes. This revelation not only challenges previous apprehensions but also adds a new layer to our understanding of COVID-19’s multifaceted impact on organ health.
A Glimpse into the Research
The study, a retrospective longitudinal multicenter cohort analysis, looked into the long-term kidney outcomes of patients hospitalized with COVID-19-associated AKI. With a sample size of 9,624 hospitalized patients spanning from March 2020 to June 2022, the research aimed to compare these outcomes against those of patients with AKI related to other illnesses, including influenza. The findings were eye-opening: COVID-19 AKI survivors had a significantly lower adjusted hazard ratio for major adverse kidney events (MAKE), including mortality and worsened kidney function, compared to those with AKI from non-COVID causes.
Understanding the Impact
The implications of these findings are manifold. For healthcare professionals, this research offers a crucial insight into managing and prognosticating for patients with COVID-19-related kidney issues. The lower risk of long-term kidney function decline and mortality in COVID-19 AKI survivors suggests a somewhat more optimistic outlook than previously thought. However, the study, as highlighted by F. Perry Wilson, MD, MSCE, of Yale School of Medicine, also underscores the necessity for ongoing research into the effects of COVID-19-specific therapeutics on kidney function trajectory.
Challenges and Considerations
Despite the positive news, the study acknowledges certain limitations, such as potential unmeasured confounders that might affect the longitudinal trajectory of eGFR and the impact of various renoprotective medicines during follow-up. This calls for cautious optimism and emphasizes the need for replication in broader cohorts. Additionally, the inability to adjust for social determinants of health due to data limitations presents a challenge that future research must address to fully understand the long-term outcomes for COVID-19 AKI survivors.
In conclusion, while the battle against COVID-19 continues, this study sheds light on a particularly dark corner of concern regarding post-recovery complications. It brings a message of hope, backed by data, to those who have faced the daunting challenge of COVID-19-related acute kidney injury. As we move forward, let this finding remind us of the resilience of the human body and the importance of ongoing, nuanced research in our journey to understand and conquer this virus.
link